Worldwide, people on the front lines have been working around the clock to contain the spread of COVID-19. With the United States experiencing the worst surge of the pandemic this holiday season, nurses, physicians, and other health professionals have their hands full. This is their story.
Inequitable access to health care has long been a challenge in the United States. Even before the COVID-19 pandemic struck, the system was plagued by exorbitant prices, lack of insurance coverage, and significant health disparities based on race, income, and ZIP codes. Compared with other developed economies, the U.S. has the highest health care expenditures, yet that investment is not reflected in its outcomes. It has lower life expectancy than the average of the OECD (the group of the world’s richest economies), as well as lower levels of health care coverage.
Now, the COVID-19 virus has cast into sharp relief the extent of the weaknesses of the health care system in the U.S. and how social determinants of health can affect outcomes in entire communities. COVID-19, which has claimed the lives of more than 300,000 Americans and counting, has been the test of a lifetime for the American health care system.
To truly put this into perspective, the United Nations Foundation spoke to front-line workers around the country who are carrying out their jobs amid waves of COVID-19. From a firefighter/EMT simultaneously responding to fires — a byproduct of another deep-rooted challenge, the global fight against climate change — and fielding medical calls, to a nurse practitioner providing guidance on health services to the most vulnerable segments of her community, we will be featuring Americans whose experiences illustrate the urgency of equitable access to quality health care, and why we must #UniteforHealth now.
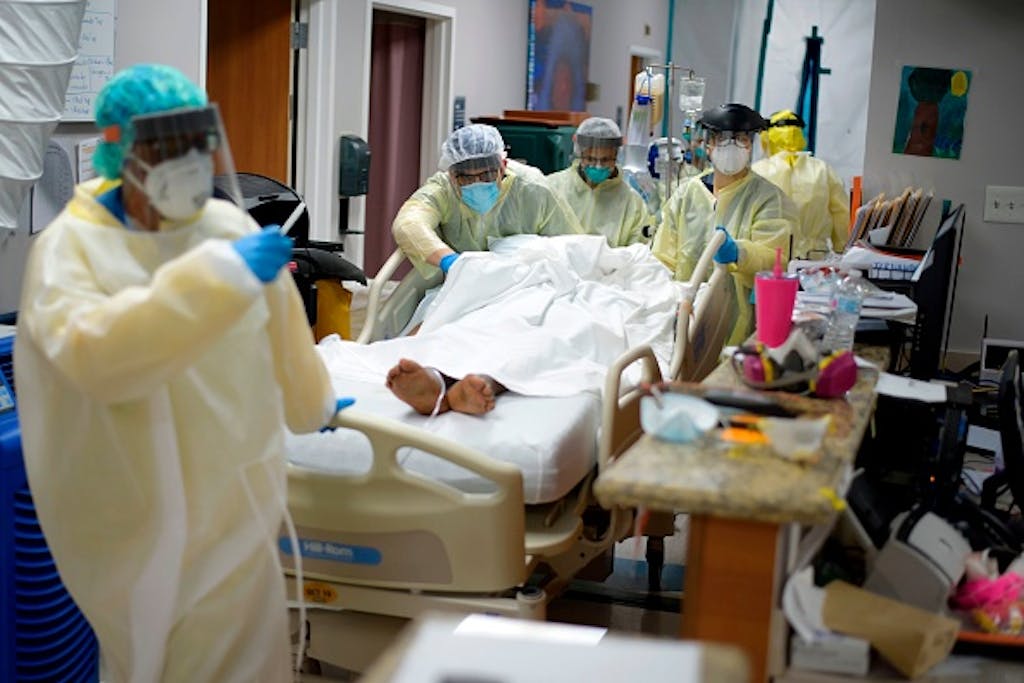
MEET ANH NGUYEN
Anh Nguyen is an emergency room physician working at Houston Methodist Hospital, one of the busiest hospitals in Texas. By the second week of December, the COVID-19 positivity rate of people who have tested for the virus in the county had spiked to 9.8%, up from 5.5% in October. We talked to Nguyen about what it’s like to work in an ER setting during a global emergency; the importance of preventive care; and how to address apathy toward the virus.
Describe your job and day-to-day duties on the front lines of COVID-19.
I‘m an ER doctor, so no shift is the same. Every single day is an environment of controlled chaos. I never know what‘s going to walk in the door — it could be someone who‘s zero to someone who‘s a hundred and we just have to take care of everybody as best as we can.
Houston Methodist is the largest tertiary care center [the highest critical care level possible] in the state and essentially serves as a receiving center for all of Texas, including advanced COVID-19 cases. We’re doing a lot of experimental treatments, and we’re one of the first academic medical centers in the country to treat patients with convalescent plasma therapy. From the very beginning of the pandemic, we have been seeing COVID-19 patients. Currently we have hundreds admitted in our hospital system and see dozens in the ER daily.
What makes the community where you work unique?
We’re in urban Houston, and serve mostly adults. Our patients are very complex, as we have a large transplant, heart, stroke, and cancer program. Houston is very diverse, which is awesome — you can get any food that you want anywhere! We receive people from every part of the socioeconomic spectrum, from the very affluent — the Bush family used Houston Methodist as their hospital — to the underserved, including homeless populations.
What have your experiences in this community taught you about the importance of equitable health access?
Equitable health access is vitally important and makes an impact in your life from the moment you are born. Even before the pandemic, people who have the ability and means to have a healthy lifestyle are more able to avoid preventable conditions such as obesity, diabetes, hypertension, or lung disease. These are all risk factors that make you more vulnerable for doing poorly once you contract COVID. If you’re already behind in terms of health education or access to health care, and you have totally uncontrolled diabetes or asthma, or you haven’t seen a primary care doctor in decades, you’re going to do worse with COVID.
We try to do what we can in the ER, but we have so little time and no relationship with patients. A huge part of my job is educating patients and answering their questions. I have COVID-19 patients who’ll ask me: “Well, why can’t you give me something to make it go away?” or “Don’t I need to stay in the hospital?” This type of education is just less accessible if you’re underserved. If my patients don’t have a safe home or reliable food on the table, I can’t possibly expect them to know where to go to get tested, or whether to even come into the hospital in the first place. There have been huge public health education efforts, but the criteria and protocols are changing daily, making it almost impossible for people to keep up.
Once patients contract COVID-19, health disparity and socioeconomic status still play a huge role in their long-term outcome. I can keep a patient in the hospital and give them all the treatment they need, and they get better and go home, but they still need follow-up for the lungs, the heart, the brain, etc. They need to be able to comprehend safe isolation practices, concerning signs at home that should prompt return to the hospital, how to buy a pulse oximeter [a small device to measure blood oxygen levels], and other basic monitoring skills. Half of my patients cannot quarantine effectively and protect their families because they don’t have the space to do so. I try to tell people to isolate in a bedroom and bathroom by themselves, or stay away from the elderly and very young — but some of them are primary caregivers to their children and elderly patients, or simply do not have the means and space to be alone. The battles are harder for underserved patients from the very beginning to the very end.
It must be quite difficult to educate the population about such a new, rapidly evolving virus. What are some of the most misunderstood aspects of COVID-19?
I think the most frustrating thing for me is not having much to offer patients who are being discharged. A simple cure simply doesn’t exist right now. Not only that, it’s hard to build trust with a patient in the ER, because I don’t know them and I have such a short time with them. They have long-term relationships with their primary care physicians, but it’s not the same case for me. I want to communicate to them that I’m not holding anything back — if I had a treatment, I would give it to them. But I don’t. Some people ask for antibiotics, for example, but that’s not helpful. Or they’ll read about new drugs online or about experimental trials, but not every hospital has every experimental drug. Even if we did, it would be indicated for certain populations and wouldn’t be appropriate for all patients.
Another frustrating thing that we are constantly educating patients about is transmission. People mistakenly presume it’s impossible to get the virus if they don’t have a known exposure, or if they’re asymptomatic. They tell us, “There’s no way I could have it. I haven’t been around anyone who has it.” I wish I could re-emphasize that point over and over and over again: You don’t have to have a known exposure. At this point, community spread is so prevalent that most of my patients have no idea where they got the virus.
It seems like we’ve reached a level of apathy where if you don’t know someone personally who’s gotten the virus, then it does not seem as real or relevant to you. How can you address this mentality?
This apathy is the very reason COVID-19 continues to survive! It needs people to transmit it! For example, if I were the last person on Earth to have COVID and I isolated effectively, the pandemic would end with me.
Perhaps the most effective way that I’ve been able to address this mentality is to remind people how they would feel if they infected their loved ones. If you get apathetic, think about how you would feel if you gave it to your son, your daughter, your parents, your coworkers, or your grandparents. Sometimes, people will specifically ask me, “I have this trip planned. Do you think I should go?”
If you get apathetic, think about how you would feel if you gave it to your son, your daughter, your parents, your coworkers, or your grandparents.
Anh Nguyen
Emergency Room Physician
I tell them that they could go, but if they came back and infected their children or parents, would the trip be worth it? I think that does make people stop and think twice, and even change their mind.
On a similar note, tell us about a challenging moment you’ve had on the job during this pandemic.
Challenging moments are a daily occurrence with COVID. People who work in the ER are famously very tough and emotionally strong, but we are all struggling right now. It is difficult to faze seasoned ER doctors and nurses because we are used to seeing horrific things every day, but this is new and tough even for us. The moral injury of having to watch people die alone without loved ones cuts the soul as much as a pediatric death. Patients are so lonely and starved for attention, and they don’t get any interaction except for us.
Another challenge is the mental energy required to protect ourselves. Every single time a patient codes — meaning when their heart stops beating — we all have the instinct to rush into the room. It’s second nature, like if you saw somebody drowning, you would jump in and save them. But I have to remind my nurses and staff to stop and put on their PPE [personal protective equipment] first. These advanced cases have horrible mortality — when a patient with COVID-19 codes, the chances of us getting them back are much lower than a regular patient who codes. It’s tough to have to put aside our nature or instinct and protect ourselves first. Watching somebody suffer and not being able to help right away weighs on a lot of our staff.
It must be devastating to watch colleagues get infected. How do you take care of your own health while being constantly exposed?
I try to be as careful as I can, but not everybody can be perfect all the time. I’m always wearing my PPE, but sometimes I touch my face without thinking about it or my phone. It’s so mentally draining having to wear PPE 24/7 day in and day out. We are fatigued, we are humans, and we simply cannot live like this forever. I used to go to work and sit and chat with my colleagues, sip coffee and relax at the desk. That does not happen anymore. Everyone is so cautious now, and it’s hard to see your friends as possible vectors of infection that can get you ill.
Everyone is so cautious now, and it’s hard to see your friends as possible vectors of infection that can get you ill.
Anh Nguyen
Emergency Room Physician
The nighttime routine when I get home is also exhausting. Some shifts I end really late, sometimes as late as 3 a.m. or a full overnight when I get home at 7 a.m. I don’t want to take a shower — I want to go to bed! But I have a young daughter, so I have to get undressed outdoors, pop my clothes in the laundry, take a shower, and then I can see my family. That adds extra time to an already long day. It’s incredibly hard for me to come in and have my daughter run towards me for a hug or a kiss and have to bypass her to wash and sanitize myself.
Can you point to something that makes you hopeful or motivates you to keep going under these tough circumstances?
I’ve been so proud of how our hospital and colleagues pivoted and changed our normal protocols. We recognized the danger and quickly shifted our operations to make things safer not only for patients and visitors, but for all front-line staff including valet, security, environmental services, etc.
It is also very uplifting to see patients who come back from near death and being mortally ill. I usually only see people once so it’s hard for me to follow up on cases. I remember one of the very first cases of COVID that I intubated in the ER and put on a ventilator. He was in the hospital in a coma for months. He was eventually put on a tracheostomy and discharged to rehab and came back to the ER five months later for a minor complication of his breathing tube. I couldn’t believe how well he recovered. We had come so far in learning about the disease and he had come so far in his recovery. It was very encouraging to see.
How has the COVID-19 experience changed you as a doctor? What will you remember 5, 10 years down the line?
There’s been a lot of moral injury from this pandemic that will take me years to recover from. The days are long and they are draining. It is emotionally exhausting to see hundreds of patients mortally ill and then go home from the hospital and see people at bars, clubs, and having giant parties. It is devastating to tell a patient I am going to have to put them to sleep and on a ventilator knowing they may never wake up. I see the fear in their eyes. But out of every storm there are positive notes and people making a difference. It has been an honor and a pleasure to collaborate with my colleagues worldwide, sharing treatment plans and advice from one epicenter of the pandemic to another. It has been a first in my lifetime to see the development of a vaccine at lighting speed. Humans are adaptable and I am confident we will get through this pandemic. The vaccine has been an early Christmas present for me, and I am cautiously optimistic that we are seeing the light at the end of the tunnel.
This holiday season, let us recognize the essential workers who are tirelessly working every day so we can be safe during this pandemic. They provide lifesaving care to those in need — often in precarious conditions. We are all safer and stronger when we #UniteforHealth.





